Memory changes linked with aging often appear subtle during early clinical stages of dementia. Family members may notice misplaced objects, repeated questions, or confusion during routine tasks, yet daily independence can remain largely intact. In many primary care settings, these signs resemble fatigue, medication effects, depression, or ordinary aging patterns. Diagnostic pathways therefore stretch across years. Multiple appointments, scattered observations, and incomplete symptom histories often slow recognition of progressive cognitive decline across routine healthcare encounters, and delayed specialist referrals occur.
Subtle Cognitive Changes Often Dismissed
Early dementia often enters quietly, through small breaks in routine rather than obvious disability. A wallet turns up in the freezer, an appointment time gets mixed up, and the same story is told twice at dinner. In primary care, these details may surface at the end of a visit meant for hypertension refills or joint pain, then disappear behind urgent problems.
Time pressure shapes the conversation. Diabetes, heart failure, sleep apnea, and chronic lung disease can fill a 15 minute slot, leaving cognitive concerns loosely documented or postponed until safety is at risk, missed doses, driving mistakes, or unpaid bills. Quick screening tests have value, yet they can miss early change. A person may perform well in a quiet exam room, then struggle at home with multi step tasks, banking, or transit routes. The result can look reassuring on paper while daily life grows harder.
Reports from family and friends can sharpen the picture, but they often arrive late. Mild forgetfulness is easy to label as normal aging, and embarrassment keeps some people silent. Clues then scatter across settings, a pharmacist noting confusion at the counter, a clinic nurse hearing repeated questions by phone, a clinician seeing only fragments for weeks.
Symptom Overlap With Other Medical Conditions
Cognitive changes linked to early dementia can look almost identical to problems clinicians see every day. Sleep disruption can blunt attention. Depression can slow thinking and reduce initiative. Thyroid disorders, low vitamin B12, anemia, uncontrolled diabetes, dehydration, and infection can all cloud memory and processing speed. For safety, most clinics check these possibilities first.
A typical visit starts with vague complaints, persistent tiredness, trouble focusing, and feeling "slower" at work or at home. Basic lab work may point to anemia or a B12 deficiency. Treatment follows, then repeat blood tests, dose changes, and another review a few weeks later. If thinking remains off, it can be hard to tell if recovery simply needs more time or if something else is developing.
Medications often muddy the picture. Older adults frequently take several medicines prescribed by different clinicians. Sedatives, certain allergy medicines, strong pain medicines, and some bladder medications can cause confusion or short-term memory problems. Deprescribing takes planning and careful monitoring, since abrupt changes can trigger falls, withdrawal symptoms, or uncontrolled pain.
Mood adds another layer. Depression can mimic dementia on brief screening tests. Referral for counseling or antidepressants may come first. Specialist assessment often arrives later, after months of tracking patterns, paperwork, and long wait lists.
Fragmented Observation Across Daily Life
Cognitive decline often becomes visible in the messiness of everyday life, not in an office visit. Early changes may show up at the supermarket, with a familiar list suddenly hard to follow, or at the kitchen table, when balancing a checkbook turns into guesswork. A recipe can start to feel unfamiliar, with steps skipped or repeated.
Patterns are usually spotted at home first. A partner may hear the same question asked several times in one evening. Adult children may find unopened mail, late notices, or a calendar filled with crossed out appointments. Many families chalk this up to stress, fatigue, or ordinary aging, and the signal stays quiet.
Medical records rarely capture these moments unless someone brings them in. Appointments tend to center on pain, blood pressure, breathing, or lab results. Clinicians rely on examples from relatives or caregivers to understand function between visits, and without that detail, the drift can look like isolated slips.
Home care staff sometimes notice red flags during check ins, missed insulin doses, mixed up pill organizers, or meals that do not match dietary plans. Even then, a single incident proves little, so teams watch for repetition before pushing for specialist evaluation. Outside the home, banks may flag unusual withdrawals, and pharmacies may see early refill requests. Each contact adds a piece to the picture.
Diagnostic Testing Requires Time and Repeated Evaluation
Confirming dementia involves more than one office visit. Neurological conditions affecting memory develop gradually, and diagnosis requires evidence of persistent decline. Clinicians therefore rely on repeated assessments. Initial evaluation usually includes a detailed history, medication review, and physical examination.

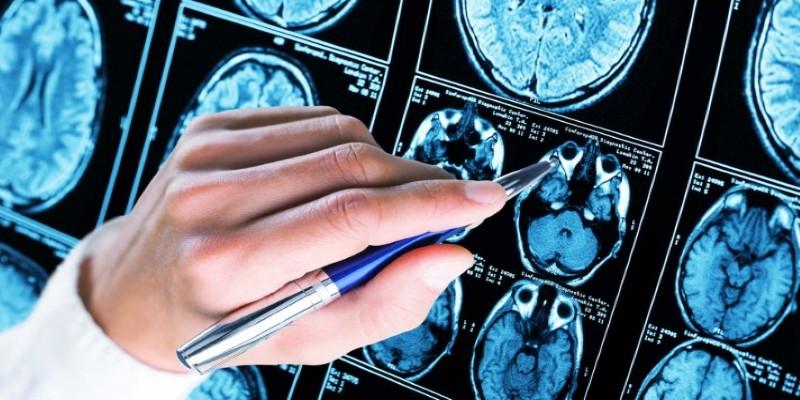
Laboratory testing checks for metabolic or nutritional causes of cognitive difficulty. Brain imaging may follow. Magnetic resonance imaging often reveals structural changes such as hippocampal shrinkage or vascular injury, yet early disease sometimes produces subtle findings.
Neuropsychological testing provides deeper insight. These evaluations measure memory, attention, language, problem solving, and visual processing. Testing sessions can last several hours. Results help distinguish dementia from normal aging patterns or mood-related cognitive changes. Even with thorough testing, physicians may monitor symptoms across time before confirming a diagnosis.
A patient might return after six or twelve months for repeat assessment. Worsening performance across visits provides clearer evidence of neurodegenerative disease. This cautious approach protects patients from premature labeling. Memory complaints carry social and emotional consequences.
Employment decisions, driving privileges, and financial management may change after diagnosis. Clinicians therefore gather consistent documentation before final conclusions. Healthcare systems also influence timing. Specialist shortages, insurance approvals for imaging, and referral coordination add delays. Each administrative step lengthens the path between the first symptom and the confirmed diagnosis.
Conclusion
Early dementia rarely appears as a single clear signal. Small memory lapses, attention problems, or planning difficulties blend with common health concerns. Clinical evaluation unfolds slowly as physicians rule out reversible conditions and observe changes across time. Family reports, home observations, and specialist testing gradually form a clearer picture. Diagnosis may take several years, not from oversight, but from careful confirmation of a progressive neurological condition that develops quietly within daily life.











